Oncology Adjuncts
Immune Surveillance & Targeted Cellular Support
Advanced Oncology Adjuncts and Immune Surveillance
Video Training — Group 10: Oncology Adjuncts
Overview
This module explores one of the most highly specialized, elite classes of supportive medicine: Oncology Adjunct Peptides. These therapeutics shift the clinical paradigm from purely destroying cancer cells (which damages healthy tissue) to instructing the body to either recognize hidden threats or directly trigger programmed cell death in malignant tissue while sparing healthy infrastructure. CRITICAL COMPLIANCE NOTE: Peptide use in oncology is strictly adjunctive and complementary. Strict collaboration with a patient's oncologist is mandatory. These are not standalone curative therapies.
Group Overview Infographic
Visual reference for all therapeutics in the Oncology Adjuncts group
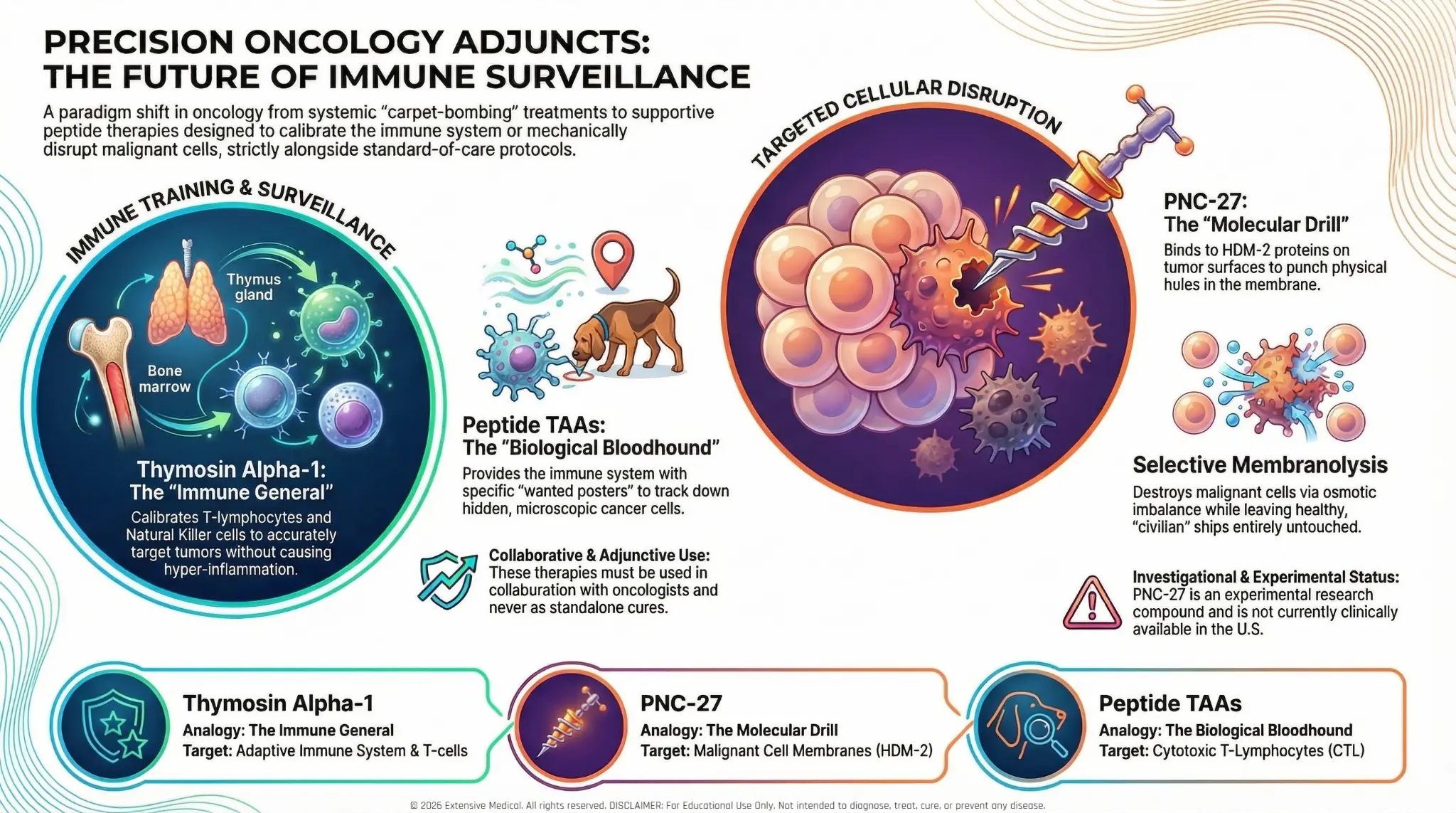
© 2026 Extensive Medical. All rights reserved. For educational use by licensed healthcare practitioners only.
IMPORTANT: All oncology adjunct peptides discussed in this module are strictly adjunctive and complementary to standard-of-care oncology treatment. They are not standalone curative therapies and should never be presented as replacements for conventional oncology care. Strict collaboration with a patient's oncologist is mandatory before initiating any adjunctive peptide protocol.
Therapeutics in This Group
Thymosin Alpha-1
TA-1 — Oncology Immune Modulator
Mechanism of Action
A naturally occurring 28-amino-acid peptide from the thymus gland. In oncology settings, acts as a powerful precision modulator of systemic immunity — maturing T-lymphocytes, increasing NK cell activity, balancing TH1/TH2 responses, and uniquely inducing apoptosis in certain cancers (melanoma, non-small cell lung cancer) through the PTEN tumor suppressor gene.
Target System
Adaptive immune system, thymic networks, and tumor suppressor pathways
Clinical Use
Used globally as a critical oncology adjunct to protect against chemotherapy-induced immunosuppression and to maintain immune surveillance capability during and after treatment.
Key Benefits
- Preservation of immune function during chemotherapy
- Documented survival improvements in clinical trials
- T-lymphocyte maturation and NK cell activation
- Apoptosis induction in certain cancer types
Key Differentiator
A true immune modulator — makes the immune system highly active and vigilant without causing a hyper-inflammatory cytokine storm that could harm a fragile oncology patient.
The Analogy
"TA-1 is the elite training instructor for the body's military academy. Cancer and chemo close the academy. TA-1 re-opens the doors — organizing, training, and equipping the cellular defense team with better strategy, radar, and weapons."
PNC-27
Experimental Membrane-Active Anti-Cancer Peptide
Mechanism of Action
An experimental, synthetic, membrane-active anti-cancer peptide engineered to seek out and bind specifically to HDM-2 protein, which is overexpressed on the surface of cancer cells but absent on healthy cells. This binding creates pores in the cancer cell membrane, leading to direct, targeted cell death (necrosis).
Target System
Cancer cell membranes — HDM-2 protein targeting
Clinical Use
Investigational compound — not clinically available in the United States. Researched for its potential to directly kill cancer cells while sparing healthy tissue.
Key Benefits
- Highly selective cancer cell targeting
- Direct membrane disruption of cancer cells
- Spares healthy cells
- Novel non-immunological mechanism
Key Differentiator
Works through a completely different mechanism than immune-based therapies — directly disrupting cancer cell membranes rather than training the immune system to attack them.
The Analogy
"PNC-27 is the biological assassin with a specific target list. It carries a wanted poster (HDM-2 binding domain) and only attacks cells displaying that exact marker — leaving all healthy cells untouched."
Peptide Vaccine TAAs
Tumor-Associated Antigens
Mechanism of Action
Synthetic peptide fragments of tumor-associated antigens (TAAs) — such as LY6K or CDCA1 — that are uniquely overexpressed by the patient's cancer. When injected, antigen-presenting cells are explicitly exposed to these markers, triggering a potent CD8+ T-cell and Cytotoxic T-Lymphocyte (CTL) immune response specifically trained to hunt down and destroy cancer cells bearing those exact markers.
Target System
Adaptive immune system — CD8+ T-cell and CTL response against specific tumor antigens
Clinical Use
Investigational therapy — used in clinical trial settings for patients with tumors that have known, identifiable, overexpressed antigen markers. Specifically designed to prevent cancer recurrence and microscopic metastasis.
Key Benefits
- Creation of long-term, highly specific immune memory
- Potential prevention of cancer relapse
- Potent, localized CD8+ T-cell attack
- Personalized specificity to individual tumor markers
Key Differentiator
Extreme, personalized specificity — while TA-1 puts the entire immune army on high alert, Peptide Vaccine TAAs provide the exact biological coordinates and description of the specific enemy target.
The Analogy
"Peptide Vaccine TAAs act like giving an immune bloodhound a piece of the suspect's clothing to sniff. You are giving the immune system the exact biological 'wanted poster' of the tumor — once the bloodhounds have that precise protein signature, they will track down those specific cancer cells anywhere in the body."
Medical Disclaimer: The information on this page is provided for educational and informational purposes only and is not intended as medical advice, diagnosis, or treatment. Statements regarding peptides and related compounds have not necessarily been evaluated by the U.S. Food and Drug Administration (FDA), and no claim is being made that any product or therapy referenced is FDA approved for the uses discussed. Always consult your licensed healthcare provider before starting, stopping, or changing any treatment, supplement, medication, or wellness protocol. Read our full Medical Disclaimer.
